This fact sheet is for anyone who is considering IVF or is about to start treatment. It explains the overall treatment process and describes what happens in the laboratory during an IVF cycle.
What is IVF?
IVF stands for In vitro fertilisation – which literally means fertilisation ‘in glass’. The name comes from the fact that in the early days, the fertilisation of eggs with sperm outside of the body used to be done in glass test tubes. The term IVF is now commonly used to mean the whole treatment process of creating a pregnancy in this way.
How much does IVF cost?
At Life Fertility Clinic in Brisbane we offer Bulk Billed or Full Service IVF. Your out-of-pocket cost for Bulk Billed IVF is around $1,100 – this is the lowest cost IVF available in Queensland. Detailed cost information for Bulk Billed IVF, or Full Service IVF Treatment can be found here.
Is IVF suitable for me?
IVF may be the best treatment option for couples who are having difficulty getting pregnant or cannot establish a pregnancy naturally.
Whether infertility or low fertility is because the woman cannot produce suitable eggs or the man cannot produce suitable sperm, or a combination of both, there are various ways to increase the chances of a successful pregnancy through IVF by controlling the body’s systems with medications and enhancing the biological processes in the laboratory.
Generally speaking, IVF can help women of child-bearing age and sometimes beyond but the pregnancy success rate for women using their own eggs does decline quite steeply after age 40. See separate fact sheet on Age and fertility.
Singles and same sex couples may also often choose to get pregnant in this way as IVF can be used in conjunction with donated eggs and sperm and also surrogacy.
Step 1: Stimulating egg development
Normally a woman’s ovaries release a single mature egg each month but in IVF treatment we stimulate the ovaries to develop more follicles (which contain the eggs) to produce a greater number of eggs. This means there is more chance of achieving a healthy embryo to transfer back into the uterus.
Hormones:
In a natural cycle, the growth of the follicles is stimulated by a hormone called ‘follicle stimulating hormone’ (FSH). When the follicle is mature, another hormone, called luteinising hormone (LH) causes release of the egg from the follicle (ovulation).
In an IVF cycle, we use artificial versions of FSH and LH to stimulate your ovary to produce multiple follicles and also to control the timing of egg release (ovulation). The process is called ‘controlled ovarian hyperstimulation’ (COHS). Medications are also used to switch off or reduce your own hormone signals and prevent them from interfering with the process.
You may be asked to take these hormones in various ways such as by a daily nasal spray or by injections. FSH is usually a daily injection, which you administer yourself after instructions from the IVF nurses.
Ultrasound monitoring:
Soon after FSH treatment has started, we monitor the response of your ovaries and the growth of follicles with ultrasound scans. The ultrasound technique involves gently placing a probe into the vagina. This is normally painless and takes only a few minutes. Results of the scans will allow the doctor to adjust your medication, if needed, to improve follicle development. We may also test your blood to monitor oestrogen levels (a hormone produced by the follicles).
Occasionally this stimulation treatment has to be stopped and your treatment postponed if the ovary does not respond or seems to be over-responding.
Step 2: Collecting the eggs
The trigger:
When the ultrasound scan shows that a number of the follicles have reached a diameter of 17mm, we administer another ‘trigger’ hormone which helps the eggs to mature and to be released by mimicking the LH surge that triggers ovulation in a normal menstrual cycle. The trigger may be given by injection or as a nasal spray. 36 hours after the trigger injection or spray, before the eggs are naturally released from the follicles, you will have a procedure to collect the eggs. This procedure is called egg retrieval or egg pick-up (EPU).
Egg pick-up procedure:
The trigger is usually given late in the evening and you will have an appointment for your EPU about 36 hours later. Your Nurse Coordinator will give you detailed instructions on when to stop the stimulation medications and when to use the trigger.
You must not eat or drink for six hours before your egg collection procedure.
You will be asked to come to the Life Fertility Clinic IVF theatre about an hour before the time of your of your procedure, where you will speak to one of our scientists and the IVF nurses. Our friendly theatre staff will do the admission paperwork and prepare you for the egg collection. EPUs can be done under local anaesthetic or sedation. Your fertility specialist will advise you which is best for you. If you are having sedation, you will meet the anaesthetist just before the procedure who will sedate you for about 30 minutes.
We collect your eggs via your vagina, using the ultrasound probe (as used during scanning) to guide a fine needle into the follicles. The follicles are drained by suction and flushing and a scientist will identify and isolate the eggs from the follicle contents.
When the procedure is over, the recovery nursing staff will take care of you and the Life Fertility Clinic nurses will tell you how many eggs were collected.
Most people are ready to leave the clinic 1-2 hours following the egg collection. You will need someone to collect you from the hospital as you shouldn’t drive for 24 hours and you should rest for the remainder of the day.
In the meantime, your eggs are transferred to the IVF laboratory and held in a culture medium ready for insemination with sperm 3-5 hours later.
Step 3: Collecting the sperm
The man will be asked to produce a semen sample around the time of the egg collection. There is a private room for this purpose at the clinic. Alternatively if you live within an hour’s travel time of the Life Fertility Clinic, the semen sample may be collected at home and delivered to the clinic for the scheduled time. We recommend that the man does not ejaculate for between two and seven days before producing this sample.
In circumstances where the man cannot be available to produce a fresh semen sample, we can arrange to freeze a sample before the egg collection.
If the man has previously been found not to have sperm in his semen even though they are being produced in his testis, he will need to have a procedure called Percutaneous Epididymal Sperm Aspiration (PESA) or Testicular Sperm Aspiration (TESA) to surgically retrieve sperm. Both of these procedures can be done through Life Fertility Clinic and will be arranged in advance (see separate fact sheet on PESA/TESA).
Life Fertility Clinic can also arrange for donor sperm if needed. Please discuss this with the IVF doctor and nurse coordinator before you start your IVF treatment.
Step 4: In vitro fertilisation and embryo culture
Insemination:
Once the laboratory has received the semen sample (or a sample of frozen sperm has been thawed), the scientists separate normal swimming sperm from the semen.
For standard IVF, this prepared sperm is used to inseminate the eggs by leaving them in culture dish together overnight. To have a good chance that the eggs will be fertilised by this method, we need a large number of normal sperm.
If the number of sperm is too low for standard IVF, or they are not of sufficient quality, we can use another method called ‘intra-cytoplasmic sperm injection’ (ICSI), where a single sperm is injected into each egg (see separate fact sheet on ICSI).
Fertilisation check:
Regardless of the insemination method we have used, we must examine the eggs under a microscope the following day to see if they have fertilised. If an egg has fertilised, the male and female genetic material are visible as two spherical bodies in the egg (Fig.1).
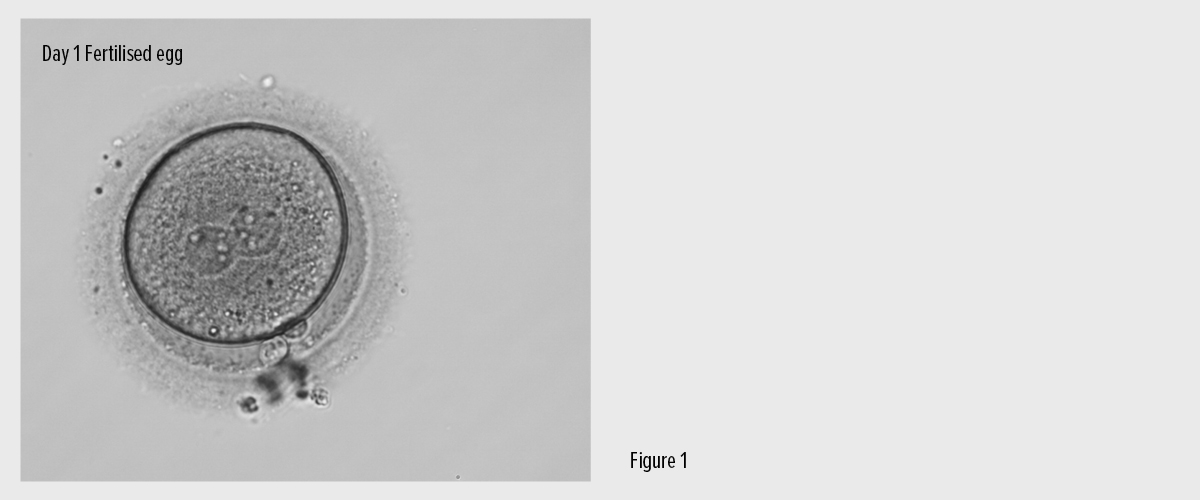
Our scientist will contact you at this stage (Day 1) to let you know your fertilisation results. For about 5% of patients who have eggs collected, fertilisation fails. Sometimes this is due to an unexpected problem identified with the eggs or sperm but sometimes there is no obvious reason.
Embryo development:
The fertilised egg is a single cell which then begins to divide. By day 3, most embryos are somewhere between 5 and 8 cells (Fig. 2).
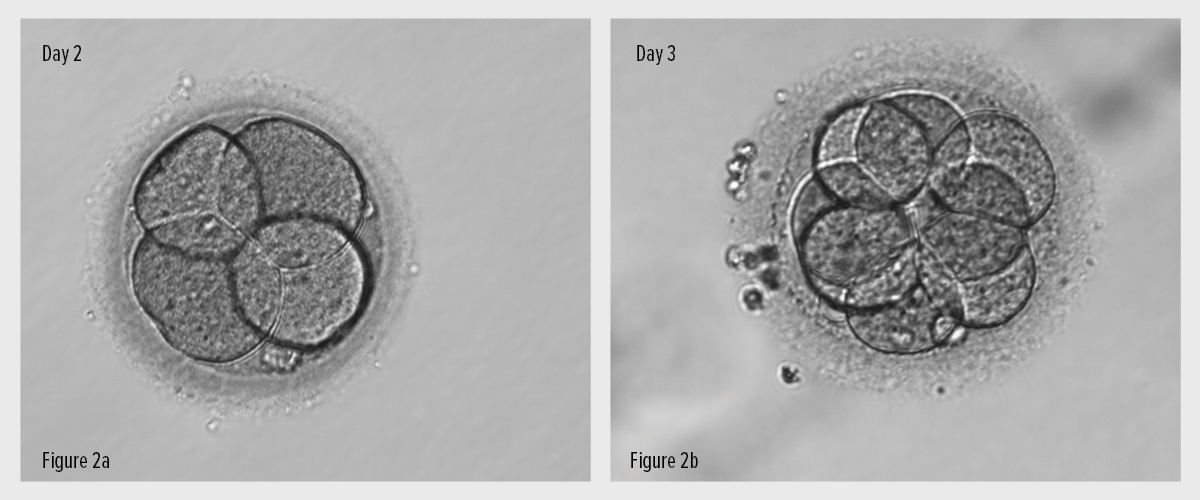
From day 3 onwards, the cell numbers increase and the cells begin to rearrange themselves, starting to differentiate into different types. By day 5, some of the embryos will reach a stage of development called a blastocyst (Fig. 3).
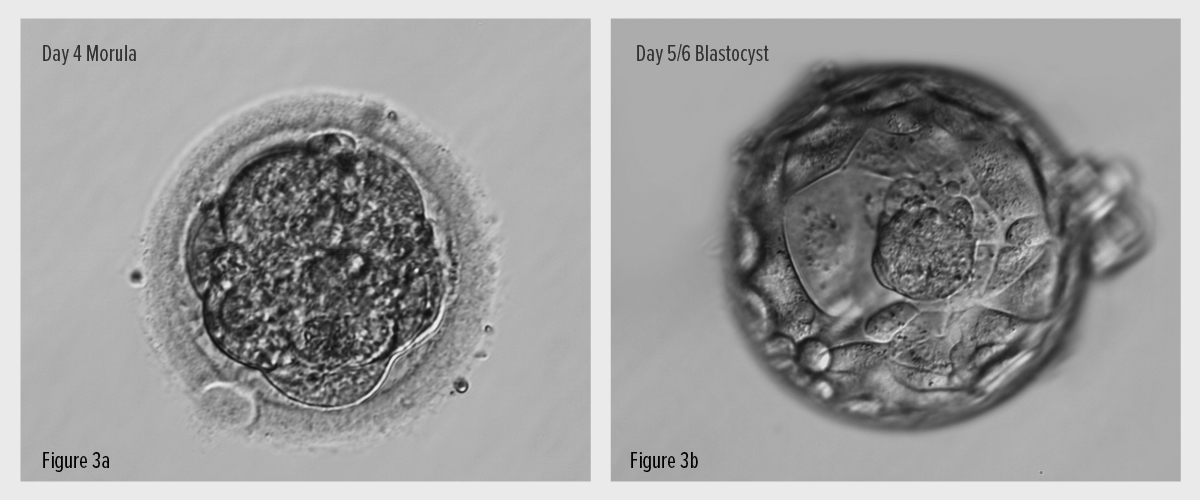
A scientist checks the embryos every day and assesses and records their progress and quality.
Step 5: Embryo transfer and freezing
Embryo transfer:
At Life Fertility Clinic, we usually transfer embryos on day 5 after fertilisation, when they are at the blastocyst stage (see separate fact sheet on blastocyst culture). Your IVF specialist will advise you if your embryos should be transferred sooner.
The embryo transfer involves placing the embryo(s) into the uterus using a thin plastic tube called a transfer catheter.
The clinician inserts a speculum into the vagina (as for a pap smear) and locates the cervix (the entrance passage to the uterus). A scientist uses a syringe to pick up the embryo(s) and place them into the tip of the catheter. The catheter is then passed through the cervix into the uterus and the embryo(s) is placed in the uterus.
The process lasts only a few minutes and does not normally require an anaesthetic. You will be asked to have a full bladder so that the clinician can view the embryo transfer using an abdominal ultrasound scan.
After the embryo transfer, the Nurse Coordinator will explain your after-care medications and the timing of your pregnancy test.
Embryo Freezing:
If you have more good quality embryos than you need, they can be frozen for future use. All embryos are cultured in the laboratory until day 6 in case any further embryos can be cryopreserved at this stage.
For some patients a fresh embryo transfer is not planned for immediately after the EPU. Instead the clinician may ask the laboratory to freeze all suitable good quality embryos at the blastocyst stage (day 5 and 6) with the plan to thaw and transfer an embryo in a subsequent frozen embryo transfer (FET) cycle. Your IVF doctor will discuss this with you in advance if we think this is the best plan for you.
Step 6: Pregnancy test and follow-up
We will order a pregnancy blood test for 11-14 days after the embryo transfer. The blood test measures the hormone human Chorionic Gonadotropin (hCG), which is produced by the early pregnancy. Please wait until the advised date to have your test as the hormones used during the cycle can lead to false readings if you test too soon.
Some women experience bleeding or spotting before their pregnancy test. This is not necessarily a period and it is important that you continue to take any prescribed medications until you have spoken to your Nurse Coordinator or fertility specialist.
If the test is positive, we will order a repeat blood test to confirm the result. If you are on medication to support the endometrial lining, it is important that you continue to take it.
We will arrange an ultrasound examination within the next two to three weeks. Once an ultrasound confirms the presence of a healthy fetus, the IVF doctor will congratulate you and discuss your plans for pregnancy care. If you live outside the Brisbane or region, we can arrange telephone follow-ups.
If the pregnancy test is negative, we will tell you which medications to stop and when. Your period may take 1-2 weeks to start and may be slightly heavier than normal. If you have been taking progesterone it can delay your period, even if you are not pregnant.
A negative test is always very disappointing and we encourage you to take advantage of our free counselling service if you would like to discuss your responses.
When you are ready, please make another appointment with your Life Fertility Clinic doctor to review your IVF cycle and plan future treatment. Although our procedures and pregnancy rates are amongst the best, sometimes it does take more than one treatment cycle to be successful. That can be a daunting thought but our new parents tell us it’s all worth it in the end!
Contact Life Fertility Clinic
The friendly and professional team at Life Fertility Clinic are happy to answer any other questions you may have about the IVF process.
